Since COVID-19 was declared a global pandemic in March, its accompanying symptoms — “fever, cough, shortness of breath, loss of taste or smell” — have practically been etched in our brains. However, we forget another shared occurrence between COVID-19 patients: their inevitable feeling of isolation. Consider two COVID-19 patients with differing backgrounds: Paul Dewyse, a 57-year-old Michigan resident and a father to three, and Ernesto Castro, a 37-year-old care worker. As a double lung transplant recipient, Dewyse already had experience staying in the hospital several times due to chronic lung issues, but this case was different. The mandatory social isolation from the real world coupled with the intrusion into his personal life from the online world left him with an unimaginable amount of emotional stress. Because his case was one of Michigan’s first two cases, news outlets trivialized his case down to one of “an adult man from Wayne County with recent domestic travel”, inadvertently doxing him for the whole world to judge. In the other case, 35-year-old Ernesto Castro, treated at the UCHealth Medical Center of the Rockies in Loveland, spent seven days in a medically induced coma for COVID-19. Recalling his feelings after he woke up, Castro said that “the hardest part was that no visitors were allowed in the hospital. I wanted my girlfriend to hold my hand. I wanted my mom to tell me everything is going to be okay.”
However, we forget another shared occurrence between COVID-19 patients: their inevitable feeling of isolation.
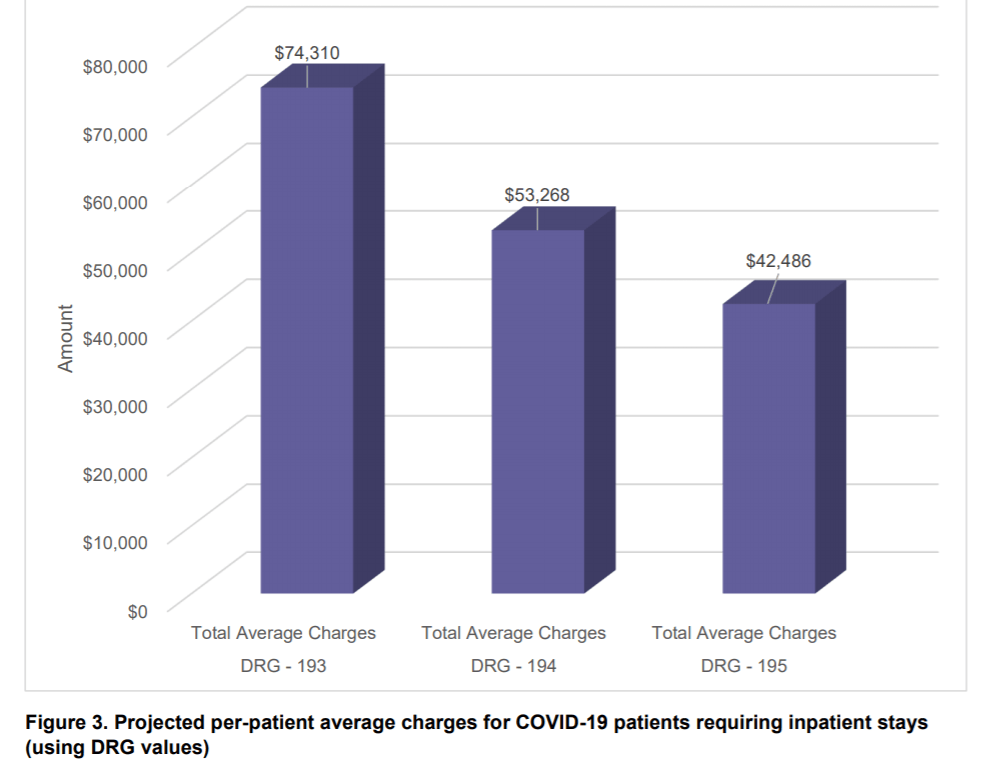
Stuck in arguably the most complex healthcare system in the world, U.S patients have always had trouble tracking their bills, insurance, and treatment plans due to unknown administrative costs. When we now add social isolation and unfamiliarity with COVID-19 to this existing mess, patients can’t help but feel absolutely powerless in the hospital. Out of the 4 million cases of COVID-19 in the U.S since January, we have seen a general trend of psychological and financial distress for hospitalized patients. Multiple studies have shown that patients in quarantine experienced more long-term psychological problems than those who weren’t. Now, with many COVID-19 patients already showing signs of anxiety, depression, and stress in the hospital, we can expect many of them to similarly experience the same long-term emotional damage from being in quarantine. From a study done on the psychological impact on quarantine, researchers found that there were multiple causes (or stressors) during quarantine that possibly led to these damages: fear of infecting others, frustration and boredom, inadequate supplies, and inadequate information. Even after quarantine, the financial stressor of having to pay the hospital bills possibly exacerbated these psychological issues. Based on previous hospitalizations for respiratory infections, the independent nonprofit FAIR Health projects that the cost for hospitalizations could range from over $21,000 to $38,755 for patients with employer insurance, with the patients spending about $1,300 to $1,464 out of pocket. What’s even worse is that, for the uninsured who will be hospitalized (approximately 670,000 to 2 million people), we can plausibly expect astronomical prices of at least $42,486 to $74,310. Because two-thirds of the uninsured are members of low-income families who are more susceptible to getting COVID-19, we can expect to see tremendous difficulties for these families in trying to navigate the healthcare system to get additional financial aid.
The National Cancer Institute defines a patient advocate as “a person who helps guide a patient through the healthcare system.” Examples of their work include helping patients communicate with their healthcare providers so they get the information they need to make decisions, helping them get financial support, and working with insurance companies and employers. Some patients may be able to have a relative or close friend take the time to do research and be their personal patient advocate or pay a professional to be their patient advocate.
While there are a few nonprofit patient advocacy groups that have developed over the past decades that do help less privileged patients, we have yet to see reform that can create a long-lasting impact…
However, many patients, specifically those in poor communities, aren’t privileged enough to afford either of these options. And while there are a few nonprofit patient advocacy groups that have developed over the past decades that do help less privileged patients, we have yet to see reform that can create a long-lasting impact on these communities. To get some insight into the effects of patient advocacy on COVID-19 patients from an individual perspective and a reform-based perspective, I interviewed Caitlin Donovan, the senior director and spokesperson for the National Patient Advocate Foundation and the Patient Advocate Foundation.
The Advocacy Process
When people normally think of patient advocacy, they tend to associate a patient receiving aid on an individual basis, but that’s only one half of it. For example, the Patient Advocate Foundation (PAF) and the National Patient Advocate Foundation (NPAF) are sister organizations. The former deals with individual patients, offering free specialized support on a case-by-case basis, while the latter deals with the national reform that can improve our health care system’s equity, access, affordability, and quality of care.

For individuals looking to receive a patient advocate, Donovan recommends that people start out deciding which kind of aid they’d like to receive. “There are two ways that people can look at it. On one hand, you can have someone help you professionally, who would be able to help you over the phone but can’t go to the doctor’s office with you, ” said Donovan. “ On the other hand, a patient may want someone who can be with them at the doctor’s office to help facilitate important conversations with the doctor, who are more likely to be a family friend or a loved one.” However, in both cases, Donovan recommended seeking an advocate “who is responsible, diplomatic yet assertive, and trustful because you are ultimately letting them deal with your personal health”.
The patient advocates in the PAF would fall in the professional category, specifically serving patients with chronic, life-threatening illnesses. However, there are a variety of other patient advocacy nonprofits that serve different purposes; Needy Meds provides patients with prescription drug assistance, Pulse Center for Patient Safety focuses on patient safety and takes on patients that are survivors of medical injuries. For the patients who qualify to be served by the Patient Advocacy Foundation, there are a variety of services that they can receive: case management, co-pay relief, etc. Case management is usually the most sought-after service for the PAF, as it provides one on one assistance, helping patients appeal for denied services or find available financial support systems.
Case managers have taken on an even larger role since the onset of COVID-19, as they also aid patients who have been hospitalized for COVID-19 or have had their chronic illness directly/indirectly worsened by COVID-19. A few examples of these new services include connecting patients to COVID-19 specific programs that address loan deferrals, accessing unemployment benefits, and evaluating whether a patient’s insurance covers COVID-19 testing, telehealth, and treatment. In addition to case management, as of May 20, 2020, the PAF has allocated a COVID Care Recovery Fund for eligible patients in need of non-medical day to day costs of living expenses due to their diagnosis, such as food expenses, utility bills.
For patients that don’t qualify for either case management or for the COVID Care Recovery Fund, the PAF has provided a plethora of resources under the COVID Care Resource Center, which includes updates on legislation being passed, websites to relief funds, and checklists to help prepare one for a COVID-19 hospitalization. The COVID-19 Planning Tip Sheet, one of the many checklists, provides an extensive list of important tasks patients normally would neglect in thinking about hospitalization for COVID-19, including “three action steps for a patient to plan out their care” and essential items to bring to a hospital stay.
Donovan highlighted two points on the list that she recommended everyone consider before going to the hospital: a phone and charger and an assigned medical decision maker. She noted that, with COVID-19, many “shared experiences have been outcries from caregivers, such as spouses and children, whose loved ones are in the hospital and they aren’t allowed to visit, so their phone becomes their lifeline.” Not only do phones help caregivers keep in touch with the patient, but they also allow caregivers to stay in touch with providers via Facetime, which more efficiently facilitates conversation between the hospital providing the treatment, the doctor, the patient, and their caregiver. This is especially important when we consider HIPAA (The Health Insurance Portability and Accountability Act of 1996), which prevents providers from sharing information with anyone who isn’t the patient. Although HIPAA acts in the patient’s best interest to protect their basic right of privacy, the pandemic has created a dilemma in which patients might not have the mental or physical capacity to make important decisions but caregivers are also not allowed to be at the hospital to help them make these decisions, making a phone and an assigned medical decision maker absolutely crucial.
Many “shared experiences have been outcries from caregivers, such as spouses and children, whose loved ones are in the hospital and they aren’t allowed to visit, so their phone becomes their lifeline.”
Caitlin Donovan
Lastly, since some states don’t provide patients with a telephone, the responsibility is placed upon the patients to prepare their own phone and charger. For example, Arizona only recently passed a waiver on its previous rule that stated that its hospitals must provide access to a phone to its patients. One would assume that, especially during these times, hospitals would prioritize patients and their rights.
However, Donovan actually mentions this as one of the biggest misconceptions: “patients think that being hospitalized for COVID-19 will be like going to the hospital under normal circumstances, but hospitals are focused on saving the greatest number of people, even if it means that someone will die who normally would not”.
For high-risk patients, this future is extremely bleak, as they will be in the center of subjective decisions made by medical professionals on whether their life is worth saving over another patient’s and, for low-risk patients, this also means that hospitals will be able to neglect their rights in order to save the lives of the high-risk patients, placing the onus of education onto each patient. While the Arizona waiver may seem like an anomaly, if more hospitals nation-wide are experiencing difficulties implementing their emergency plans and suffering from surge capacity, we can expect to see a greater number of states signing waivers limiting patient’s rights for the greater good of the hospital. Ultimately, this places more pressure on the patient to be prepared and, until we can see permanent reform being placed onto the healthcare system, patient advocates and being prepared are a patient’s best bet in getting the best quality care they can get at the hospital.
This is the first article in a two-part series about patient advocacy. The second installment will focus on the national reform and policy coming from the NPAF and other patient advocacy groups in regards to COVID-19.
Edited by Akila Muthukumar, Anu Zaman
Thanks for your personal marvelous posting! I really enjoyed reading it, you happen to be a great author.I will be sure to bookmark your blog and will often come back in the foreseeable future. I want to encourage one to continue your great posts, have a nice evening!
LikeLike
I appreciate your wp template, exactly where would you down load it from?
LikeLike
Hello! We are using a theme named Canard.
LikeLike